Biosynthesis of ZnO NPs based Resin Nanocomposites: A Sustainable Oral Health Care Solution
1Department of Chemistry, Ramnarain Ruia Autonomous College, L.N. Road, Matunga (East), Mumbai, Maharashtra, India
2Tata Institute of Fundamental Research, Mumbai, India, Adjunct Professor, Ramnarain Ruia Autonomous College, Matunga (East), Mumbai, Maharashtra, IndiaCorresponding Author E-mail:shravaniwadekar996@gmail.com
Download this article as:
ABSTRACT:Dental caries is a highly prevalent chronic disease globally, emphasizing the need for sustainable and biocompatible materials in restorative dentistry. This study presents the green synthesis of zinc oxide nanoparticles (ZnO NPs) using Cassia fistula leaf extract and their incorporation as nanofillers in resin nanocomposites comprising UDMA, GMA, APTES, and CQ. This formulation serves as a cost-effective substitute for Bis-GMA based products. The formation of ZnO NPs was confirmed using UV–Vis spectroscopy, FTIR, FESEM, HRTEM, XRD, and DLS techniques. Resin nanocomposites with varying compositions of ZnO NPs were synthesized and evaluated for mechanical properties including tensile strength, flexural strength, and compressive strain, and compared to TiO₂ NPs based composites. The optimal formulation with 0.15 g ZnO NPs showed a tensile strength of 1415.53 gf, flexural strength of 16.26 gf, and compressive strain of 71.84% at 0.10 g. Results indicate that ZnO NPs with UDMA, GMA, and APTES offer a sustainable, efficient, and economical alternative to conventional dental materials. Further investigations include cytotoxicity evaluation via MTT assay on fibroblast cell lines (triplicate experimental run), in vivo testing, antibacterial and antifungal studies against common oral pathogens, and assessment of synergistic effects with other nanoparticles to enhance efficacy.
KEYWORDS:Compression Strength; Flexural Strength; GMA; Resin Nanocomposites; Tensile Strength; ZnO NPs
Introduction
Dental caries remains one of the most common oral health problems worldwide, affecting individuals across all age groups. According to the World Health Organization (WHO), more than 3.5 billion (around 45%) people globally experience toothache or related complications, making it a pressing public health concern1. The human oral cavity harbours complex microbial communities that often develop resistance to conventional antimicrobial therapies. If left untreated, dental caries can progress from enamel to dentin, leading to inflammation, infection, necrosis, and ultimately, tooth loss2. Furthermore, poor oral health has been linked to systemic conditions such as cardiovascular disease, diabetes, chronic headaches, auditory complications, and adverse pregnancy outcomes. These associations highlight the urgent need for restorative materials that are not only cost-effective but also capable of preventing infection and promoting long-term oral health3.
Historically, dental materials such as amalgam, cements, and conventional resin-based composites have been employed for restorative procedures4. However, these materials present several drawbacks, including inadequate adhesion, marginal leakage, biofilm accumulation, and biocompatibility concerns. Notably, amalgam fillings, which have been used for over a century, have been largely phased out due to their mercury content, which has been associated with neurological and renal toxicity5. Additionally, amalgam surfaces tend to promote bacterial colonization, leading to secondary degradation and compromised restoration integrity.
In response to these limitations, nanotechnology has emerged as a transformative solution in dentistry. The incorporation of metal and metal oxide nanoparticles into resin-based composites has shown considerable promise in improving antibacterial performance, mechanical strength, and aesthetic properties6. Among the various nanoparticles explored, zinc oxide nanoparticles (ZnO NPs) stand out due to their excellent antibacterial, antifungal, and physicochemical properties. ZnO NPs are notably efficient in disrupting bacterial cell membranes, diminishing biofilm formation, avoiding secondary cavities, exhibiting superior adhesive properties, and maintaining non-toxicity while being ecologically benign.7
Crucially, the biosynthesis of ZnO NPs using plant-based extracts offers a green and sustainable alternative to traditional chemical and physical synthesis methods8,9. In this study, we utilized the aqueous extract of Cassia fistula leaves to synthesize ZnO NPs through an eco-friendly approach that eliminates the need for toxic reagents and high-energy processes as previously reported10. These biosynthesized ZnO NPs were then integrated into a resin nanocomposite matrix composed of glycidyl methacrylate (GMA), urethane dimethacrylate (UDMA), and 3-(aminopropyl) triethoxysilane (APTES), along with the photo-initiator camphorquinone (CQ), to develop a novel dental restorative material. The resulting ZnO NP-based resin nanocomposite exhibits enhanced antibacterial efficacy, superior mechanical stability, and improved adhesion that makes it a viable, sustainable solution for oral healthcare11,12. By combining biocompatibility with eco-conscious synthesis and advanced functional performance, this material represents a promising step toward comprehensive, cost-effective dental care solutions that meet both clinical and environmental goals.
Materials and Methodology
All chemicals used in our study were of analytical reagent (A.R.) grade with a reported purity of 100%. UDMA, APTES, CQ, and GMA were obtained from Sigma-Aldrich, Mumbai, India. Polyvinyl alcohol (PVA), acetone, glycerol, distilled water, titanium dioxide nanoparticles (TiO₂ NPs), and commercial zinc oxide powder (ZnO powder) were procured from SRL, Mumbai, India. A commercially available dental composite (Dentsply Spectrum Composite Syringe Restorative Kit; Shade: A2; Batch No.: 2003000436) manufactured by Dentsply Sirona were used as a control.
Cylindrical and disc-shaped Teflon molds (diameter: 6–10 mm; thickness: 1–2 mm; depth: 2 mm) were used for sample preparation. Photopolymerization was conducted utilizing a light-curing apparatus (Model: Woodpecker Mini S, Woodpecker, China) with a 3W high-power blue LED (wavelength range: 420–480 nm; light intensity: 1000–1200 mW/cm²; weight: 150 g).
Synthesis of ZnO NPs
ZnO NPs were synthesized by a previously documented green synthesis process, in which the plant extract served as both the reducing and stabilizing agent, as formerly reported earlier10. The resulting nanoparticles were characterized through various hyphenated analytical techniques including ultraviolet-visible (UV-Vis) spectroscopy, Fourier transform infrared spectroscopy (FTIR), powder X-ray diffraction (PXRD), field emission scanning electron microscopy (FESEM), high-resolution transmission electron microscopy (HRTEM), and energy dispersive X-ray analysis (EDAX) as established in earlier studies10.
Preparation of ZnO NPs-Based Resin Nanocomposites
ZnO NPs, prepared using the aforementioned method10, were used to prepare the resin nanocomposites. Initially, 0.05 g of ZnO NPs were dispersed in 5 mL of APTES in an Erlenmeyer flask. The mixture was stirred using a magnetic stirrer (Remi, 150 W, dimensions: 200 × 225 × 185 mm, speed range: 15–1500 rpm, stirring capacity: up to 800 mL) at 30–40 °C for 20–30 minutes at 500rpm until complete dispersion and solubilization of the ZnO NPs was achieved. Additional APTES was added accordingly if the dispersion appeared dry. In a separate beaker, 0.4 mL of UDMA and 0.6 mL of GMA were mixed without heating using a magnetic stirrer for 20–30 minutes at 500rpm. This UDMA-GMA mixture was then added to the ZnO NPs–APTES solution and stirred at 50–80 °C until a homogeneous, slightly semisolid consistency was obtained and thereafter 0.01g of CQ was added and stirred vigorously to activate the solution. Subsequently, 0.2mL–0.5 mL of glycerol was added and stirred without heating to yield a viscous solution.
Separately, 0.1 g of PVA was dissolved in 10 mL of distilled water and stirred at 60 °C for 30 minutes, followed by cooling to obtain a uniform solution. A Petri dish was placed on a magnetic stirrer maintained at 60–70 °C, into which the semisolid ZnO NPs–APTES–UDMA–GMA-CQ mixture was introduced. A small amount of the prepared PVA solution (1% w/v) was added, and the entire mixture was blended thoroughly using a spatula to obtain a cohesive semisolid suspension. The final nanocomposite suspension was cast into disc-shaped PTFE-Teflon moulds (2 mm depth, 2 mm thickness, 10 mm diameter). The moulds were air-dried and subsequently photo-cured using a light-curing device positioned 2 cm above the samples. After curing, the specimens were removed from the moulds using a syringe needle. Additionally, resin nanocomposite formulations containing 0.10 g and 0.15 g of ZnO NPs were prepared following the same procedure. These samples were subjected to mechanical characterization, including tensile, flexural, and compressive strength analysis. A schematic representation of the fabrication process is illustrated in Figure 1.
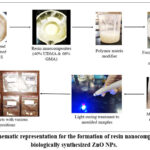 |
Figure 1: Schematic representation for the formation of resin nanocomposites using biologically synthesized ZnO NPs. Click here to View Figure |
Results
Characterization of ZnO NPs Using Various Analytical Techniques
The synthesized ZnO NPS exhibited unique structural and morphological attributes, validated through hyphenated analytical techniques as reported earlier10.
Tensile Strength Analysis of synthesized resin nanocomposites:
Tensile strength analysis was conducted on the resin nanocomposites, incorporated with varying concentrations of ZnO NPs and TiO₂ NPs, as summarized in Table 1. ZnO NPs based resin nanocomposites (Samples A–F) present the tensile strength results containing ZnO NPs and TiO₂ NPs at concentrations ranging from 0.05 g to 0.15 g. For ZnO NPs (Table 1, Samples A–C), a moderate tensile strength was observed with 0.05 g. However, increasing the concentration to 0.10 g resulted in the lowest tensile strength across the samples. A marked improvement was noted at 0.15 g, where the maximum tensile strength reached 1415.53 gf (gram force). In contrast, TiO₂ NPs (Table 1, Samples D–F) exhibited a different trend. At 0.05 g, the tensile strength was moderate, increasing significantly to a peak value of 1789.0 gf at 0.10 g. However, further increasing the concentration to 0.15 g led to a sharp decline in tensile strength, dropping to 228.09 gf.
Table 1: Tensile strength of ZnO NPs and TiO2 NPs based resin nanocomposites with varying concentration.
| Sample number | Specifications of resin nanocomposites | Sample composition | Concentration | Tensile strength (gf) |
| A |
All resin nanocomposites prepared using 0.4 mL UDMA + 0.6 mL GMA |
ZnO NPs | 0.05 g | 463.731 |
| B | 0.10 g | 313.901 | ||
| C | 0.15 g | 1415.5306 | ||
| D | TiO2 NPs | 0.05 g | 1693.81 | |
| E | 0.10 g | 1789.0 | ||
| F | 0.15 g | 228.09 |
Flexural strength analysis of synthesized resin nanocomposites:
The flexural strength for ZnO NPs based resin nanocomposite (Table 2, Samples A- C) increases with increasing concentration for 0.05 g to 0.15 g from 10.00 gf to 16.26 gf whereas, the opposite trend is observed with TiO2 NPs based resin nanocomposite (Table 2, Samples D-F), decreasing with increasing concentration for 0.05 g to 0.15 g from 25.57 gf to 11.14 gf.
Table 2: Flexural strength analysis of ZnO NPs and TiO2 NPs based resin nanocomposites with varying concentration.
| Sample number | Specification resin nanocomposite | Sample composition | Concentration | Flexural strength (gf) |
| A |
All resin nanocomposites prepared using 0.4 mL UDMA + 0.6 mL GMA |
ZnO NPs | 0.05 g | 10.00 |
| B | 0.10 g | 13.38 | ||
| C | 0.15 g | 16.26 | ||
| D | TiO2 NPs | 0.05 g | 25.57 | |
| E | 0.10 g | 20.87 | ||
| F | 0.15 g | 11.14 |
Compression strength analysis of synthesized resin nanocomposites:
ZnO NPs based resin nanocomposite samples (Table 3, Samples A-C): Demonstrated a highest peak compression percentage of 71.84% for 0.10 g, succeeded by 71.75% for 0.05 g and 71.49% for 0.15 g, respectively.
TiO2 NPs based resin nanocomposite samples (Table 3, Samples D-F): A contrary tendency is noted for TiO2 NPs resin nanocomposites. The maximum compression percentage is 71.83% for 0.15 g, succeeded by 71.58% for 0.10g and 71.50% for 0.05 g.
ZnO NPs and TiO2 NPs based resin nanocomposites (Table 3, Sample G, H): Represents samples with 0.1 g and 0.15 g each of ZnO NPs and TiO2 NPs, respectively, resulting in two distinct concentration samples. The highest percentage of compression, 71.67%, is noted in resin nanocomposite samples containing 0.15 g each of ZnO NPs and TiO2 NPs, followed closely by samples with 0.10g each of the same components at 71.58%.
Spectrum samples: 0.01 g each of ZnO NPs, TiO2 NPs, and commercial ZnO powder were combined individually with 0.1 g each of a commercial spectrum sample and subjected to a compression test as detailed in (Table 3, Samples I-K). The highest percentage of compression recorded was 28.05% for ZnO powder, 100.04% for ZnO NPs, and 19.95% for TiO2 NPs.
Table 3: Compression testing of ZnO NPs and TiO2 NPs based resin nanocomposites, including hybrid and commercial spectral samples.
|
Sample number |
Sample composition | Specification of resin nanocomposite | Concentrations | Maximum compression load (Newton) | Maximum compression strain (%) |
| A | ZnO NPs
|
All resin nanocomposites prepared using 0.4 mL UDMA+ 0.6 mL GMA | 0.05 g | 13.75 | 71.75 |
| B | 0.10 g | 13.87 | 71.84 | ||
| C | 0.15 g | 06.81 | 71.49 | ||
| D | TiO2 NPs
|
0.05 g | 37.70 | 71.50 | |
| E | 0.10 g | 18.58 | 71.58 | ||
| F | 0.15 g | 09.21 | 71.83 | ||
| G | ZnO NPs + TiO2 NPs | 0.1 g + 0.1 g respectively | 05.80 | 71.58 | |
| H | ZnO NPs + TiO2 NPs | 0.15 g + 0.15 g respectively | 14.88 | 71.67 | |
| I | TiO2 NPs | – | 0.01 g TiO2 NPs in 0.1 g of spectrum
(commercial) |
1684.00 | 19.95 |
| J | ZnO NPs | – | 0.01 g ZnO NPs in 0.1 g of spectrum (commercial) | 1532.76 | 100.04 |
| K | ZnO Powder | – | 0.01 g ZnO Powder in 0.1 g of spectrum (commercial) | 33.18 | 28.05 |
Discussion
Tensile strength analysis
Both ZnO NPs and TiO2 NPs have superior mechanical characteristics at appropriate concentrations13,14. Effective dispersion of nanoparticles enhances the interfacial interaction between the nanoparticles and the metacrylate of nanocomposites, hence improving tensile strength15,16. Nonetheless, the agglomeration of nanoparticles leads to diminished mechanical strength owing to decreased interfacial contact17-19. ZnO NPs demonstrate superior tensile strength at elevated concentrations (0.15 g) in contrast to TiO2 NPs, which display comparable findings at a reduced concentration of 0.05 g (Table 1, Sample A-F). The differences arise from the elevated surface energy of TiO₂ NPs by interaction with air and moisture, owing to the presence of hydroxyl (–OH) groups on their surface20. TiO2 NPs efficiently absorb water molecules from the environment, which then dissociate on the surface to generate terminal and bridging hydroxyl groups, thereby enhancing their surface reactivity21. These groups establish strong interfacial interactions with the resin matrix, facilitating effective stress transfer and enhancing resistance to failure under external loads22-23. As the concentration of TiO2 NPs rises to 0.15g, agglomeration may occur, interrupting the light-curing process24-26. Moreover, TiO2 NPs possess a high refractive index (2.6-2.9), resulting in enhanced light scattering during the curing process. This dispersion may lead to partial polymerization, resulting in porosity (defects / voids) inside the resin matrix. Conversely, ZnO NPs exhibit superior performance at elevated concentrations (0.15 g) owing to their enhanced dispersion and strong interfacial interaction with the resin matrix, facilitating more efficient stress distribution27-28. Moreover, ZnO NPs possess a lower refractive index compared to TiO2 NPs, resulting in less light scattering. This guarantees enhanced polymerization efficiency and inhibits the emergence of flaws such as opacity or air voids.
Flexural strength analysis
ZnO NPs have superior flexural strength at a higher concentration (0.15 g) relative to TiO2 NPs, primarily attributable to enhanced dispersion within the resin matrix and the establishment of strong interfacial bonding. This improved dispersion, facilitates efficient stress distribution, leading to enhanced flexural strength29. The reduced refractive index of ZnO NPs enhances the polymerization process, resulting in a more stable final composite. Conversely, TiO2 NPs have superior flexural strength at a lower concentration (0.05 g), but this strength diminishes as the concentration rises to 0.15g. At elevated concentrations, the aggregation of TiO2 NPs may occur, compromising the resin matrix and adversely impacting the polymerization process. The incomplete polymerization, along with the eventual formation of air gaps or defects, results in decreased flexural strength and overall mechanical performance30.
Compression analysis
ZnO NPs at 0.05 g yield a higher percentage compression as compared to TiO2 NPs, mostly due to better dispersion of nanoparticles, surface activity and strong interfacial bonds between resin composite (Table 3, Sample A). As concentration increases to 0.15 g, the compression activity decreases mostly due to agglomeration of nanoparticles (Table 3, Sample B, C). The reverse trend is observed with TiO2 NPs (Table 3, Samples D, F). When binary composites ZnO NPs are combined with TiO2 NPs with 0.1 g each, it a lower value for percentage compression than with 0.15g each. Hence, with increase in concentration the difference observed is 9.0% (Table 3, Sample G, H). This could be due to multiple factors; the co-addition may lead to differences in surface energy and particle size which may lead to weakening of the structural integrity of the composite and hence reducing matrix reinforcement31. In summary, the expected synergistic effect may not be observed with the combination of ZnO NPs and TiO2 NPs as observed using nanoparticles, alone.
However, when combined with spectrum, it shows a higher percentage compression for ZnO NPs (100.04%) and the lowest for TiO2 NPs (19.95%), attributed to the difference in resin-nanoparticles interaction32. ZnO NPs may agglomerate with the spectrum resin, leading to weaker reinforcement and more deformation with the highest percentage compression, hence showing higher flexibility (Table 3, Sample J). In contrast, TiO2 NPs show better dispersion, providing structural support and the highest compression load with low percentage compression and get deformed easily under stress (Table 3, Sample I). Moreover, when combined with ZnO powder commercially, it shows a moderate percentage compression along with the lowest compression load than the other two, implying its least ability for structural integration due to its large size and surface area33-35. This could be because commercial ZnO may not bond effectively with the commercial spectrum as effectively as with TiO2 NPs, leading to the higher deformation, though the overall strength is moderate36-38. Hence, out of three, TiO2 NPs and ZnO NPs outperformed well than commercial ZnO in restorative dental composites, with TiO2 NPs bearing maximum load and ZnO NPs with maximum flexibility.
Future Scope
Samples with more than 99% compression strain suggest their potential use in applications where flexibility is important. However, this property can be optimized by eliminating nanoparticle agglomeration and adjusting the concentration and morphological characteristics. Therefore, future studies should focus on modifying the material to enhance its suitability for restorative applications. Additionally, biocompatibility studies of ZnO NPs-based resin nanocomposites are recommended through cytotoxicity evaluation (MTT assay) and antibacterial assays to determine their minimum inhibitory concentrations (MIC), along with comparisons to TiO₂ NPs to ensure safe use39-41. These materials should also be made eco-friendly to ensure long-term stability without degradation. Recently, 3D printing has shown promising applications in restorative dentistry; hence, the prepared resin nanocomposites could be explored for 3D printing compatibility to improve both clinical and material outcomes42. Furthermore, these materials can be investigated for use in various dental fields, including endodontics, orthodontics, periodontics, implantology, cosmetic dentistry, and preventive dentistry, due to their enhanced properties and biocompatibility43. It is worth investigating the impact of nanoparticle shape (e.g., rods, sheets, spheres) on resin reinforcement behaviour. It is necessary to scale up nanocomposite synthesis using green and cost-effective methods for broader commercial applications in dental, biomedical, and structural materials. The impact of integrating antibacterial agents on the depth of cure, degree of conversion, microleakage, and bond strength to enamel and dentin, alongside their compatibility with different adhesive systems, necessitates comprehensive in vitro examination; furthermore, in situ studies are recommended to assess the influence of human saliva and the oral environment on the antibacterial, mechanical, and physical properties of resin nanocomposites44.
Conclusion
This study shows that nanoparticles concentration, refractive index, adhesive bonding, particle size, and surface energy greatly affect the mechanical properties of resin-based nanocomposites. At lower concentrations, TiO₂ NPs exhibited higher tensile and flexural strength, possibly due to good dispersion in the resin matrix. At higher concentrations, particle aggregation and surface contact led to agglomeration, reducing mechanical performance. TiO₂ NPs also demonstrated remarkable stiffness and structural stability, with the lowest compression percentage and highest compressive load among the evaluated materials.
ZnO NPs showed better tensile and flexural strength at moderate concentrations, likely due to improved nanoparticle dispersion and resin-matrix interaction. However, at slightly lower concentrations, the percentage compression was highest, indicating potential agglomeration and structural weakness. Compared to the commercial spectrum resin, ZnO NP-incorporated samples demonstrated greater compression strain with moderate compressive force, suggesting enhanced flexibility, elasticity, and better compatibility with the resin, likely aided by surface modification. In contrast, the commercial ZnO powder, composed mostly of larger particles, provided minimal mechanical reinforcement due to poor dispersion, trace impurities, and limited interfacial interaction with the resin. At higher concentrations, both ZnO and TiO₂ NPs showed increased compression strain, possibly due to particle interference and disrupted nanoparticle–resin bonding, emphasizing the necessity for meticulous tuning of nanoparticle incorporation in dental nanocomposite formulations.
Acknowledgement
The Authors would like to express sincere gratitude to the Dr. P.S. Ramanathan laboratory at Ramnarain Ruia Autonomous College, ICT (Institute of Chemical Technology) in Matunga, IIT (Indian Institute of Technology) Mumbai, and ICON labs in Navi Mumbai for characterization and data analysis. Special thanks to Dr. Heeresh Shetty from Nair Hospital for his guidance and support.
Funding Sources
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflict of Interest
The author(s) do not have any conflict of interest.
Data Availability Statement
This statement does not apply to this article.
Ethics Statement
This research did not involve human participants, animal subjects, or any material that requires ethical approval.
References
- World Health Organization, 2022. [Website]
- Femiano, F.; Femiano, R.; Femiano, L.; Jamilian, A.; Rullo, R.; Perillo, L. Eur. J. Paediatr. Dent. 2016, 17, 243.
- Comeau, P.; Burgess, J.; Malekafzali, N.; Leite, M. L.; Lee, A.; Manso, A. Materials 2022, 15, 5075.
CrossRef - Ferracane, J. L. J. Funct. Biomater. 2024, 15, 173.
CrossRef - Raorane, D. V.; Chaughule, R. S.; Pednekar, S. R.; Lokur, A. Saudi Dent. J. 2019, 31, 194.
CrossRef - Naguib, G.; Maghrabi, A. A.; Mira, A. I.; Mously, H. A.; Hajjaj, M.; Hamed, M. T. BMC Oral Health. 2023, 23, 1.
CrossRef - Bourgi, R.; Doumandji, Z.; Cuevas-Suárez, C. E.; Ammar, T. B.; Laporte, C.; Kharouf, N.; Haikel, Y. Coatings. 2025, 15, 33.
CrossRef - J., N.; K., E.; R. S. Resour. Chem. Mater. 2024, 3, 294.
- Bouttier-Figueroa, D. C.; Cortez-Valadez, M.; Flores-Acosta, M.; Robles-Zepeda, R. E. BioNanoScience. 2024, 14, 3385.
CrossRef - Wadekar, S. R.; Hate, M. S.; Chaughule, R. Orient. J. Chem. 2025, 41.
CrossRef - Ok, I.; Aykac, A. Chem. Pap. 2023, 77, 6959.
CrossRef - Matei, A.; Cernica, I.; Cadar, O.; Roman, C.; Schiopu, V. Int. J. Mater. Form. 2008, 1, 767.
CrossRef - Tiwari, A. K.; Jha, S.; Singh, A. K.; Mishra, S. K.; Pathak, A. K.; Ojha, R. P.; Yadav, R. S.; Dikshit, A. Crystals. 2022, 12, 1063.
CrossRef - Zhang, O. L.; Niu, J. Y.; Yin, I. X.; Yu, O. Y.; Mei, M. L.; Chu, C. H. Dent. J. 2023, 11, 59.
CrossRef - Chaughule, R.; Raorane, D.; Pednekar, S.; Dashaputra, R. Nanocomposites and Their Use in Dentistry. pp. 59–79, 2018.
CrossRef - Alfaawaz, Y. F.; Alamri, R.; Almohsen, F.; Shabab, S.; Alhamdan, M. M.; Ahdal, K. A.; Farooq, I.; Vohra, F.; Abduljabbar, T. Scanning. 1–9, 2022.
CrossRef - Shirkavand, S.; Moslehifard, E. DOAJ. 2014, 8, 197.
- AlGhamdi, M. A.; Alatiyyah, F. M.; Dawood, Z. H. A.; Alshaikhnasser, F. Y.; Almedarham, R. F.; Alboryh, S. Y.; Elakel, A.; Akhtar, S.; Khan, S. Q.; Gad, M. M. J. Prosthodont. 2024.
- Balhaddad, A. A.; Garcia, I. M.; Mokeem, L.; Alsahafi, R.; Collares, F. M.; De Melo, M. a. S. Bioengineering. 2021, 8, 146.
CrossRef - Hammer, B.; Wendt, S.; Besenbacher, F. Top. Catal. 2010, 53, 423.
CrossRef - Nayak, R. K.; Mahato, K. K.; Ray, B. C. Composites Part A Appl. Sci. Manuf. 2016, 90, 736.
CrossRef - Azmy, E.; Al-Kholy, M. R. Z.; Fattouh, M.; Kenawi, L. M. M.; Helal, M. A. Int. J. Biomater. 2022, 1–9, 2022.
CrossRef - Naguib, G.; Maghrabi, A. A.; Mira, A. I.; Mously, H. A.; Hajjaj, M.; Hamed, M. T. BMC Oral Health. 2023, 23, 1.
CrossRef - Khlifi, K.; Atallah, M. S.; Cherif, I.; Karkouch, I.; Barhoumi, N.; Attia-Essaies, S. Surfaces Interfaces. 2023, 41, 103279.
CrossRef - Gad, M. M.; Abualsaud, R.; Al‐Thobity, A. M.; Baba, N. Z.; Al‐Harbi, F. A. J. Prosthodont. 2020, 29, 422.
CrossRef - Alhotan, A.; Yates, J.; Zidan, S.; Haider, J.; Silikas, N. Materials. 2021, 14, 2659.
CrossRef - Pai, E.; Nayak, A.; Hallikerimath, R. B.; Ruttonji, Z.; Astagi, P.; Pokale, S. J. Indian Prosthodont. Soc. 2023, 23, 127.
CrossRef - Nguyen, T. M. T.; Wang, P.; Hsu, H.; Cheng, F.; Shieh, D.; Wong, T.; Chang, H. Mater. Sci. Eng. C. 2018, 97, 116.
CrossRef - Omar, M. H.; Amin, M. H.; Younis, H. A. Appl. Phys. A. 2022, 128, 4.
CrossRef - Dias, H. B.; Bernardi, M. I. B.; Bauab, T. M.; Hernandes, A. C.; De Souza Rastelli, A. N. Dent. Mater. 2018, 35, e36.
CrossRef - Raja, T.; Devarajan, Y.; Kailiappan, N. Discover Applied Sciences. 2024, 6, 11.
CrossRef - Vikram, S.; Chander, N. G. Eur. Oral Res. 2020, 31, 35.
CrossRef - Ferracane, J. L. Dent. Mater. 2010, 27, 29.
CrossRef - Ahuja, D.; Akhila, M. R.; Singh, A. K.; Batra, P. J. Int. Oral Health. 2024, 16, 439.
CrossRef - Kundie, F.; Azhari, C. H.; Muchtar, A.; Ahmad, Z. A. J. Phys. Sci. 2018, 29, 141.
- Almoharib, B. K.; Alshammari, O. M.; Alonazi, R. S.; Alshehri, A. A.; Alanazi, M. A.; Alqubaysi, H. A.; Alshammari, A. F.; Alzuhair, N. A.; Alenizi, A. A.; Khormi, F. A.; Alshammari, M. H.; Al-Mutairi, N. H. Int. J. Health Sci. 2023, 7, 3341.
CrossRef - Lizymol, P. P.; Vibha, C.; Deepu, D. R.; Waghmare, S. ORMO-48. pp. 211–224, 2024.
CrossRef - Duraisamy, R. Int. J. Dent. Oral Sci. 2021, 4380, 4387.
- Anzabi, R. M.; Divband, B.; Tukmachi, M. S.; Vahedifar, S.; Esmaeilzadeh, M.; Sefidan, F. Y.; Jahanbani, M.; Rafighi, A. Int. J. Dent. 2025, 1.
- Jowkar, Z.; Moaddeli, A.; Shafiei, F.; Tadayon, T.; Hamidi, S. A. Clin. Exp. Dent. Res. 2024, 10, 1.
CrossRef - Saini, R.; Vaddamanu, S. K.; Kanji, M. A.; Quadri, S. A.; Hassan, S. a. B.; Anil, S.; Shrivastava, D.; Srivastava, K. C. BMC Oral Health. 2024, 24, 1.
CrossRef - Balestra, D.; Lowther, M.; Goracci, C.; Mandurino, M.; Cortili, S.; Paolone, G.; Louca, C.; Vichi, A. Materials. 2024, 17, 1380.
CrossRef - Jeong, M.; Radomski, K.; Lopez, D.; Liu, J. T.; Lee, J. D.; Lee, S. J. Dent. J. 2023, 12, 1.
CrossRef - Algarni, A. A. Cureus. 2024.
Accepted on: 23 Aug 2025
Second Review by: Dr. Roopa Rajput
Final Approval by: Dr. B.K Sharma

















