Prostate cancer: Diagnosis, Therapeutic Interventions and Emerging Challenges
1Department of Pharmaceutical Chemistry, Sri Adichunchanagiri college of pharmacy, Adichunchanagiri university, B.G Nagar, Karnataka, India
2Department of Pharmaceutical Analysis, Sri Adichunchanagiri college of pharmacy, Adichunchanagiri university, B.G Nagar, Karnataka, India.
Corresponding Author E-mail:knp.pharma@gmail.com
DOI : http://dx.doi.org/10.13005/ojc/410208
ABSTRACT:Prostate cancer, the second most prevalent malignancy in men worldwide, is a complex disease caused by various factors like genetic, environmental, and hormonal influences. Despite progress in interpreting its pathogenesis, difficulties in reliable diagnosis and effective therapy remain. Present diagnostic instruments, such as prostate-specific antigen (PSA) testing and digital rectal examination (DRE), have limited specificity, frequently leading to overdiagnosis and unwanted biopsies. Novel biomarkers, like PCA3 and multiparametric MRI (mpMRI), have improved diagnostic accuracy, especially in detecting clinically important tumors. fortunately, these technologies continue to be underutilized in resource-limited environments. From active surveillance for low-risk instances to surgery, radiation, chemotherapy, and immunotherapy for late stages - the therapeutic methods for prostate cancer cover a wide range. Recent advancements, particularly next-generation anti-androgens and immunotherapeutic strategies, have revolutionized therapy paradigms; yet, obstacles such as medication resistance, significant adverse effects, and decreased quality of life persist. Even though active surveillance is now recognized as an effective way to reduce overtreatment; nevertheless, its execution needs rigorous methods for monitoring. The future of prostate cancer management depends on the incorporation of innovative biomarker studies, sophisticated imaging methods, and tailored treatment protocols. Despite advancements in enhancing survival rates, the advancement of more accurate and barely noticeable diagnostic and therapeutic techniques remains essential. Prostate cancer treatment must progress towards a more individualized strategy, guaranteeing optimal results while maintaining patient quality of life.
KEYWORDS:Biomarker; Chemotherapy; Diagnosis; immunotherapy; Prostate cancer (PCa); Prostate-specific antigen (PSA)
Introduction
Cancer is caused by alterations in the genetic or epigenetic composition of somatic cells and is marked by unregulated cellular proliferation that may metastasis to various regions of the body. 1 The prostate is a male auxiliary reproductive organ that is located beneath the bladder. Its principal function is to sustain essential secretions in the sperm and to maintain the viability of the sperm. Cancer that occurs in the prostate is referred to as prostate cancer. 2 Prostate cancer is the second most frequently diagnosed cancer among men across the globe. 3 Reports indicate significant racial and ethical disparities in incidence, with figures in India varying from 4.4 per 100,000 to 118.2 per 100,000 individuals. 4 After reaching the age of 50, there is a significant increase in the incidence of prostate cancer, particularly pronounced after the age of 64. 5 While the exact process that causes prostate cancer is still unknown, a number of factors appear to be involved, including age, genetic predisposition, exposure to chemicals, radiation, and environmental contaminants. Early stage of prostate cancer doesn’t show any symptoms, but the most common symptoms of prostate cancer include difficulty in urination (especially at nights), blood in urine or semen, pain in pelvic region, erectile dysfuntion, pain in testicles, etc. Androgens help in the healthy growth and functioning of prostate, and also potentially hasten the development of cancer at this time. 6 Figure 1 depicts the stage of prostate cancer according to the TNM classification method. Treatment choices and prognosis are established through accurate staging of prostate cancer using the TNM system (Tumour, Nodes, Metastasis), Gleason scores, and PSA levels. PSA values were utilized for direct staging and therapy with the TNM staging approach. 7
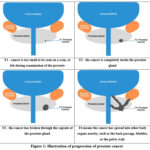 |
Figure 1: Illustration of progression of prostate cancerClick here to View Figure |
The Gleason score, developed by Dr. Donald Gleason is the predominant technique for histological assessment of prostate cancer. Grade 5 signifies the most atypical kind of dysplastic tissue, while grade 1 denotes low-degree or well-differentiated dysplastic tissue. Higher the Gleason score, the higher is its potency to spread cancer. It helps in the diagnosis of stage of cancer and better choice of treatment can be done. Various imaging modalities, including computed tomography (CT), multiparametric MRI, and technetium-99m diphosphate scintigraphy bone scans, have been employed to detect metastases and stage metastatic prostate malignancy. Multiparametric magnetic resonance imaging (mp-MRI) has shown promise in the detection, localization, staging, risk assessment, and prospective therapy choices for prostate cancer. 8
A cancer biomarker is a measurable trait that can evaluate a patient’s chances of developing cancer, regardless of the presence of symptoms. Prostate cancer management has undergone a revolutionary change with the discovery of biomarkers for screening, diagnosis and prognostication. PSA, which stands for prostate-specific antigen, is a widely used biomarker for identifying prostate cancer. To develop recommendations for prostate cancer screening, guideline statements were created based on evidence and consensus from the panel on the early detection of prostate cancer. 9
Biomarkers are important for prostate cancer because they can be used for early detection and diagnosis, risk stratification, prognostic value, treatment guidance, tracking disease progression and treating resistance prediction. The different types of biomarkers are discussed in Table 1. 10 Prostate-specific antigens are not very specific for detecting prostate cancer. This could potentially result prostate biopsies, so it’s important to find more accurate indicators for prostate cancer and/or high-risk prostate cancer. 11
Table 1: Biomarkers in Prostate cancer 12
| S. No | Biomarker | Sample type | Assay method |
| 1 | PSA(Prostate specific antigen) | Blood | Immunoassay |
| 2 | Free PSA (fPSA) | Blood | Immunoassay |
| 3 | PCA3(Prostate cancer antigen 3) | Urine | TMA(Transcription-mediated amplification) |
| 4 | Prostatic Acid Phosphatase (PAP) | Blood serum | Enzyme-linked immunosorbent assay (ELISA) or colorimetric assays |
| 5 | Androgen Receptor (AR) Variants | Blood or tumor tissue | Polymerase Chain Reaction (PCR) or Next-Generation Sequencing (NGS) |
| 6 | 4Kscore(A combined total PSA, free PSA, intact PSA, and human kallikrein 2) | Blood plasma | Immunoassays combined with a risk prediction algorithm |
| 7 | PSA Density (PSAD) | Blood and imaging (e.g., ultrasound for prostate volume) | Calculation using serum PSA levels and prostate volume measurement |
| 8 | TMPRSS2-ERG fusion | Urine | TMA(Transcription-mediated amplification) |
| 9 | EN2 | Urine | Immunoassay |
Note: Prostate-specific antigen (PSA), Multiparametric MRI (mpMRI), positive predictive value (PPV), Prostate cancer antigen 3 (PCA3), clinically significant prostate cancer (csPCA) and other biomarkers are among the techniques used to detect cancer of the prostate.
Diagnosis of Prostate cancer
Emerging carcinoma of the prostate biomarkers are improving diagnosis. 13 Figure 2 lists a few diagnostic techniques that are employed during the diagnosis process. Blood tests for prostate-specific antigen (PSA) and digital rectal examinations have been used in the detection of prostate cancer (PCa). Following the diagnostic procedure, a transrectal ultrasound (TRUS) guided biopsy was conducted. 14 Both treatment failure and the disease’s late stages at diagnosis contribute to an ever-increasing death rate. There isn’t a single test that can diagnose prostate cancer, but the standard practice is a digital rectal examination (DRE), in which a doctor wearing gloves looks into the rectum with a gloved finger to measure the prostate’s size and check for anomalies. 15
The diagnosis of prostate cancer is significantly aided by biomarkers. Today, alternative biomarkers detectable in physiological fluids offer a potential for innovation, as PSA screening has transformed the way prostate cancer was identified over 30 years ago. While missing fewer clinically important malignancies, the use of biomarkers and biomarker panels may decrease the likelihood of diagnosis without clinical significance. 16 To enhance the identification of clinically relevant prostate cancer, several novel assays and testing methodologies are being evaluated. 17
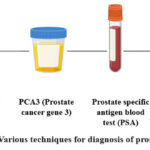 |
Figure 2: Various techniques for diagnosis of prostate cancer.Click here to View Figure |
TRUS prostate dissection
The main method used for diagnosing prostate cancer is transrectal ultrasound (TRUS). Prostate biopsy sampling with digital rectal guidance was proven to be less effective than systematic biopsy based on TRUS, which is the current standard diagnostic procedure for prostate cancer. Random TRUS biopsy has also been used to identify low-grade indolent cancers, thereby potentially overrating. 14
Prostate-specific antigen (PSA)
A significant transition has occurred due to PSA screening, as it is capable of detecting prostate cancers that are clinically relevant, which probably accounts for the decrease in prostate cancer death rates. PSA screening often uncovers low-grade conditions that are unlikely to be clinically significant during a man’s lifetime, leading to a notable overdiagnosis of these non-aggressive diseases. 18 Despite this, the PSA blood test remains the main approach for identifying prostate cancer. 15
The lack of specificity in PSA screening for prostate cancer is a primary issue, particularly when results are less than 10 µg/L. This low specificity indicates that many men may have needless biopsies performed to confirm or rule out cancer. As a result, 65-75% of men who have PSA levels ranging from 3/4 to 10µg/L do not have prostate cancer that can be detected through biopsy. To enhance specificity and decrease the incidence of unnecessary or repeat biopsies, several additional or complementary tests have been suggested. These tests include PSA, PHI, PCA3, and the 4K score. 19
Digital Rectal Examination (DRE)
Routine examination of males within the standard primary acre evaluation includes DRE. However, a study indicated that DRE may contribute less to the reduction of mortality, but instead to increase the rate of false positives that could have high rates of unnecessary invasive diagnostic testing that could cause pain, erectile dysfunction, incontinence, overdiagnosis and overtreatment of prostate cancer. 20 Rectal examinations are routinely performed to assess male voiding dysfunction, but are not useful as an initial diagnostic device for cancer. The major part of patients whose prostate cancer was diagnosed by PSA screening had normal DRE. Regardless of the PSA level, prostatic biopsy continues to be warranted in the event of probing irregularities or nodules during DRE. 14
Prostate cancer antigen 3 (PCA3)
The urine-based biomarker, prostate cancer antigen 3 (PCA3), has recently gained popularity because of its utility in identifying clinically relevant malignancies. PCA3, also termed DD3 (differential display code 3), is a prostate-specific non-coding mRNA. PCA3 expression was found in benign prostatic enlargement and normal prostate tissue, but it was absent from several normal and malignant tissues outside the prostate. 19
Additionally, the FDA authorized the progensa PCA3 test in 2012. It measures long non-coding RNA (InRNA) present in urine sediments obtained after performing three strokes of a digital rectal exam (DRE) prostate massage. Individuals with prostate cancer might exhibit levels of its expression that are as much as 80 times greater than those of people with benign prostatic hyperplasia. The progensa PCA3 test’s primary use is whether a negative biopsy should follow up on; however, the FDA only approved this indication due to the high risk of overlooking high-grade PCa (HGPCa) with a low PCA3 value. 21
Multiparametric MRI (mpMRI)
Multiparametric magnetic resonance imaging (mpMRI) has become a useful tool, especially in presurgical local T staging, due to its ability to detect tumors that biopsy could have missed and its excellent distinction of the soft tissues surrounding the prostate. 22 In recent years, multiparametric magnetic resonance imaging (mpMRI) has gained increasing popularity because of its ability to detect clinically significant cancers. 23
Prostate biopsy has drawbacks, however mpMRI offers a number of benefits when used to treat prostate cancer. In order to expedite the use of MR-targeted prostate biopsies, multiparametric MRI enables the visualization of regions likely to contain clinically relevant cancer before biopsy, allowing some men to avoid an imminent biopsy. This enables better identification and characterization of higher-risk malignancies, increased patient selection for active surveillance, and a decrease in the diagnosis of clinically unimportant diseases. Furthermore, mpMRI can be utilized to choose and track patients for active monitoring and treatment planning. 24
Challenges in diagnosis
Diagnosing prostate cancer (PCa) can be difficult because existing diagnostic techniques, such as PSA tests, digital rectal exams, and transrectal ultrasound, have limitations. Although multiparametric MRI has been proven to enhance the diagnosis of prostate cancer and is advised before conducting a biopsy, a considerable number of prostate cancer cases still go undetected by mpMRI. 25
PSA itself is a simple blood test, and there can be challenges and difficulties associated with the test and, its interpretation. The appearance of false positive and false negative rate in the test can be challenging and cause problems in the diagnosis. 26 The diagnostic performance of Digital Rectal Examination (DRE) is restricted, PSA levels vary between individuals, and traditional Transrectal Ultrasound (TRUS) is not sensitive enough. Routine PSA screening for prostate cancer is generally discouraged and is still a topic of discussion, as there is no proof that it improves overall survival rates or survival specifically from cancer. Additionally, there is a concern regarding the possibility of concern regarding the possibility of overdiagnosis and unnecessary treatments. 27 A number of non-aggressive, indolent cancers may never become life-threatening and are frequently found with PSA screening. This may lead to overtreatment and unnecessary biopsies, putting patients at risk for no therapeutic gain. 28 Numerous diagnostic instruments, such as liquid biopsies, genomic testing, and advanced imaging, are expensive and not commonly available, especially in smaller or less resource-rich medical facilities. Overdiagnosis is still possible even with all diagnostic instruments at hand. The only method to reduce the risk of overtreatment is to break the mandatory connection between diagnosis and active treatment. 7
Treatment of prostate cancer
Treating cancer is a great challenge as it depends on many factors.29–31 Patients with prostate cancer receive treatment based on the aggressiveness, health, and stage of their disease. The major treatments carried out are active surveillance, surgery, radiation, hormone therapy and chemotherapy among other modalities which is also mentioned in the figure 3. Surgery and radiation treatment are effective treatments for men with more advanced illness, such as those whose PSA levels are higher than 10ng/mL or who show palpable nodules on digital rectal examination. 32 The treatment landscape for prostate cancer has changed significantly over the last decade due to innovative therapies, enhanced diagnostic tools, advancements in next-generation sequencing, and more effective use of current drugs in the early stages of the disease. 33
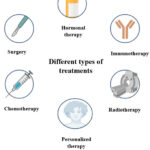 |
Figure 3: Different modes of treatment for Prostate cancer.Click here to View Figure |
 
The treatment of patient in prostate cancer is done accordingly after knowing the stage of the disease and as per that differ types of treatment methods or therapies are used. Chemotherapy, radiation, hormonal therapy and surgery are some of these treatment methods.
Active Surveillance
Active surveillance is a dynamic tactic. In the five-to ten-year time span, it has become more widely recognized as a safe treatment for favorable-risk prostate cancer. 34 Active surveillance has been shown to be the best approach for patients with low-risk malignancies or those with little time to live. The criteria for active surveillance often include suggestions based on life expectancy, health problems, illness features, side effects, and patient preferences. 35
Active surveillance involves regular monitoring of PSA levels, imaging, and repeat biopsy. It has the potential to be an affordable strategy that reduces overtreatment while maintaining quality of life. 36 Although active surveillance is a good alternative for people who want to avoid treatment adverse effects immediately, the monitoring procedures and inclusion criteria have not been standardized. 37
Surgery
Surgical intervention has shown superior oncological outcomes compared to radiation therapy, and it has been proven to improve cancer-specific survival rates and metastasis-free survival, while also decreasing the need for palliative care in contrast to observation. 38 The majority of cases high-risk locally progressed prostate cancer are recommended for surgery. The two most prevalent surgical options for prostate cancer are radical prostatectomy (RP) and pelvic lymphadenectomy (PLDN). Radical prostatectomy has generally been deferred in cases of high-risk prostate cancer due to concerns about potential side effects, including significant rates of positive surgical margins, lymph node metastases, and recurrence of prostate-specific antigen (PSA). Surgical process is, however, more beneficial than closely monitoring mortality, local progression risk, and metastatic risk, as surveillance has shown. 39
Radical prostatectomy combined with pelvic lymph node dissection has gained traction as the main treatment for high-risk localized lymphomas. This method may assist in mitigating the negative consequences associated with androgen deprivation therapy (ADT). 40
Radiation therapy
An essential component of treating cancer is radiation therapy. Radiation acts as a physical agent aimed at eliminating cells. The type of radiation utilized is referred to as ionizing radiation, as it generates ions-particles with electric charge-and transfers energy to the cells in the tissues it interacts with. This energy can either kill cancer cells directly or lead to genetic alterations that result in their destruction. Radiation can target malignant tissues in two primary methods: external beam radiation involves directing high-energy rays (such as photons, protons, or particle radiation) from outside the body towards the tumor site. This approach is the most commonly employed in clinical settings and is called External Beam Radiation Therapy (EBRT). Another mode of therapy called Brachytherapy, or internal radiation, involves applying radioactive source directly to the tumor site using sealed catheters or by inserting them within the body. Injecting radioactive pharmaceuticals into tumor site is another mode of treatment. 41
Chemotherapy
Chemo is a potential option for treating advanced prostate cancer that has been researched since the early 1980s. 42 Many chemotherapy medications have been authorized for treating prostate cancer. 43
Docetaxel was the initial chemotherapeutic drug to demonstrate a benefit in overall survival for patients with metastatic castration-resistant prostate cancer (mCRPC). 44 Every three weeks, intravenous doses of docetaxel and cabazitaxel are administered to stop tubulin depolymerization, which would otherwise cause mitotic cell division and ultimately cause cell death. 43 In 2012, enzalutamide, which is a second-generation androgen receptor inhibitor, was recognized as a chemotherapeutic option for treating prostate cancer. 15
Immunotherapy
It involves targeting cancers with the immune system and includes a wide range of therapies commonly known as immunotherapy. Immunotherapy changed the standard of care for several tumor types, profoundly affecting the treatment of metastatic cancer, although reactions have generally been difficult to predict and understand in many different forms of tumors. Prostate cancer has traditionally not responded well to the immunotherapies, though a few metastatic tumors, such as cutaneous melanoma, lung cancer and hypernephroma have dramatically responded. However, an exceptionally low percentage of patients with prostate cancer have responded very well with cellular and immunotherapy and thus, it deserves further studies. 45
The last decade has seen massive development in immunotherapy, with this treatment now being a mainstream part of treatment for patients suffering from advanced solid malignancies. Notably, patients in the past have had little to no benefits of prostate cancer immunotherapy. Due to enhanced antitumor immunity brought about by recent advancements in molecular diagnostic platforms and immune mechanism research, immunotherapy has become a desirable treatment for adenocarcinoma of the prostate, especially castration-resistant prostate cancer (CRPC). 46 The use of vaccinations to produce active immunity has long been investigated in the field of oncology. 47
Challenges in treatment
Prostate cancer is a highly varied illness, with different tumor aggressiveness and genetic makeup. This makes it difficult to forecast disease progression and distinguish between patients who need severe treatment and those who may be managed with active surveillance. 48 Some of the most common treatment options for advanced prostate cancer are immunotherapy, chemotherapy, androgen deprivation therapy (ADT), along with targeted therapy. The current challenges are to determine the optimal sequencing and mix of these medications. This is essential for people diagnosed with metastatic castration-resistant prostate cancer (mCRPC). 49
Radiation therapy and systemic treatments like androgen deprivation therapy (ADT) produce serious adverse effects such as external dysfunction, urine incontinence, and bone health problems. Managing these adverse effects while preserving patients’ quality of life remains a crucial concern. 50 Advanced treatments, such as second-generation anti-androgens like abiraterone and enzalutamide, frequently cause prostate cancer to become resistant. This resistance is caused by variety of process, including AR mutations and alternative androgen receptor signaling, resulting in poor results in late-stage disease. 12
Conclusion
There is still a significant amount of difficulties associated with the diagnosis and treatment of prostate cancer treatment. At this time, the diagnostic procedures that are most often utilized, including as the digital rectal exam and PSA testing, have a low specificity and lead to overdiagnosis with unneeded biopsies, particularly in individuals who are considered to be at low risk. Biomarkers that have recently been established, such as PCA3, as well as sophisticated imaging methods that are easily available, have contributed to an improvement in the sensitivity of the identification of clinically relevant cancers. In addition, the current treatment choices that are available today include hormone therapy, chemotherapy, radiation therapy, surgery, and immunotherapy. These kinds of treatments give a great deal of specialist care and raise the likelihood of survival in instances that are high-risk and advanced. However, more severe side effects, such as dysfunction, urinary incontinence, and other symptoms of bone loss, have a negative impact on the quality of life an individual has. In low-risk circumstances, active surveillance has been found to reduce the amount of overtreatment that occurs; nevertheless, its implementation requires stringent monitoring requirements. It is possible that some developing medications, including as immunotherapy and genetic testing, could prove to be more effective than previously thought; nevertheless, further research will be required to make the most of these treatments. Patients suffering from prostate cancer will, in the future, require care that is more effective and individualized, and in order to achieve these goals, innovation in biomarker research, imaging, and tailored therapy will be required.
Acknowledgement
All the authors are thankful to Sri Adichunchanagiri College of Pharmacy for their support throughout the work.
Conflicts of Interest
The authors declare that there are no conflicts of interest
References
- Saini, A.; Kumar, M.; Bhatt, S.; Saini, V.; Malik, A. CANCER CAUSES AND TREATMENTS. Int J Pharm Sci Res 2020, 11, 3121, doi:10.13040/IJPSR.0975-8232.11(7).3121-34.
CrossRef - Rawla, P. Epidemiology of Prostate Cancer. World J Oncol 2019, 10, 63–89, doi:10.14740/wjon1191.
CrossRef - Wasim, S.; Lee, S.-Y.; Kim, J. Complexities of Prostate Cancer. Int J Mol Sci 2022, 23, 14257, doi:10.3390/ijms232214257.
CrossRef - Kimura, T.; Egawa, S. Epidemiology of Prostate Cancer in Asian Countries. International Journal of Urology 2018, 25, 524–531, doi:10.1111/iju.13593.
CrossRef - Sankarapillai, J.; Krishnan, S.; Ramamoorthy, T.; Sudarshan, K.L.; Mathur, P. Descriptive Epidemiology of Prostate Cancer in India, 2012–2019: Insights from the National Cancer Registry Programme. Indian Journal of Urology 2024, 40, 167–173, doi:10.4103/iju.iju_27_24.
CrossRef - Barani, M.; Sabir, F.; Rahdar, A.; Arshad, R.; Kyzas, G.Z. Nanotreatment and Nanodiagnosis of Prostate Cancer: Recent Updates. Nanomaterials 2020, 10, 1696, doi:10.3390/nano10091696.
CrossRef - Mottet, N.; van den Bergh, R.C.N.; Briers, E.; Van den Broeck, T.; Cumberbatch, M.G.; De Santis, M.; Fanti, S.; Fossati, N.; Gandaglia, G.; Gillessen, S.; et al. EAU-EANM-ESTRO-ESUR-SIOG Guidelines on Prostate Cancer—2020 Update. Part 1: Screening, Diagnosis, and Local Treatment with Curative Intent. Eur Urol 2021, 79, 243–262, doi:10.1016/j.eururo.2020.09.042.
CrossRef - Barsouk, A.; Padala, S.A.; Vakiti, A.; Mohammed, A.; Saginala, K.; Thandra, K.C.; Rawla, P.; Barsouk, A. Epidemiology, Staging and Management of Prostate Cancer. Medical Sciences 2020, 8, 28, doi:10.3390/medsci8030028.
CrossRef - Wei, J.T.; Barocas, D.; Carlsson, S.; Coakley, F.; Eggener, S.; Etzioni, R.; Fine, S.W.; Han, M.; Kim, S.K.; Kirkby, E.; et al. Early Detection of Prostate Cancer: AUA/SUO Guideline Part II: Considerations for a Prostate Biopsy. Journal of Urology 2023, 210, 54–63, doi:10.1097/JU.0000000000003492.
CrossRef - Farha, M.W.; Salami, S.S. Biomarkers for Prostate Cancer Detection and Risk Stratification. Ther Adv Urol 2022, 14, doi:10.1177/17562872221103988.
CrossRef - Fujita, K.; Nonomura, N. Urinary Biomarkers of Prostate Cancer. International Journal of Urology 2018, 25, 770–779, doi:10.1111/iju.13734.
CrossRef - Jakobsen, N.A.; Hamdy, F.C.; Bryant, R.J. Novel Biomarkers for the Detection of Prostate Cancer. J Clin Urol 2016, 9, 3–10, doi:10.1177/2051415816656121.
CrossRef - Kohaar, I.; Petrovics, G.; Srivastava, S. A Rich Array of Prostate Cancer Molecular Biomarkers: Opportunities and Challenges. Int J Mol Sci 2019, 20, 1813, doi:10.3390/ijms20081813.
CrossRef - Descotes, J.-L. Diagnosis of Prostate Cancer. Asian J Urol 2019, 6, 129–136, doi:10.1016/j.ajur.2018.11.007.
CrossRef - Sekhoacha, M.; Riet, K.; Motloung, P.; Gumenku, L.; Adegoke, A.; Mashele, S. Prostate Cancer Review: Genetics, Diagnosis, Treatment Options, and Alternative Approaches. Molecules 2022, 27, 5730, doi:10.3390/molecules27175730.
CrossRef - Lomas, D.J.; Ahmed, H.U. All Change in the Prostate Cancer Diagnostic Pathway. Nat Rev Clin Oncol 2020, 17, 372–381, doi:10.1038/s41571-020-0332-z.
CrossRef - Merriel, S.W.D.; Funston, G.; Hamilton, W. Prostate Cancer in Primary Care. Adv Ther 2018, 35, 1285–1294, doi:10.1007/s12325-018-0766-1.
CrossRef - Albertsen, P.C. Prostate Cancer Screening and Treatment: Where Have We Come from and Where Are We Going? BJU Int 2020, 126, 218–224, doi:10.1111/bju.15153.
CrossRef - Duffy, M.J. Biomarkers for Prostate Cancer: Prostate-Specific Antigen and Beyond. Clinical Chemistry and Laboratory Medicine (CCLM) 2020, 58, 326–339, doi:10.1515/cclm-2019-0693.
CrossRef - Naji, L.; Randhawa, H.; Sohani, Z.; Dennis, B.; Lautenbach, D.; Kavanagh, O.; Bawor, M.; Banfield, L.; Profetto, J. Digital Rectal Examination for Prostate Cancer Screening in Primary Care: A Systematic Review and Meta-Analysis. The Annals of Family Medicine 2018, 16, 149–154, doi:10.1370/afm.2205.
CrossRef - Porzycki, P.; Ciszkowicz, E. Modern Biomarkers in Prostate Cancer Diagnosis. Cent European J Urol 2020, 73, 300–306.
CrossRef - Oliveira, T.; Amaral Ferreira, L.; Marto, C.M.; Marques, C.; Oliveira, C.; Donato, P. The Role of Multiparametric MRI in the Local Staging of Prostate Cancer. Frontiers in Bioscience-Elite 2023, 15, 21, doi:10.31083/j.fbe1503021.
CrossRef - Tan, G.H.; Nason, G.; Ajib, K.; Woon, D.T.S.; Herrera-Caceres, J.; Alhunaidi, O.; Perlis, N. Smarter Screening for Prostate Cancer. World J Urol 2019, 37, 991–999, doi:10.1007/s00345-019-02719-5.
CrossRef - O’Connor, L.P.; Lebastchi, A.H.; Horuz, R.; Rastinehad, A.R.; Siddiqui, M.M.; Grummet, J.; Kastner, C.; Ahmed, H.U.; Pinto, P.A.; Turkbey, B. Role of Multiparametric Prostate MRI in the Management of Prostate Cancer. World J Urol 2021, 39, 651–659, doi:10.1007/s00345-020-03310-z.
CrossRef - Correas, J.-M.; Halpern, E.J.; Barr, R.G.; Ghai, S.; Walz, J.; Bodard, S.; Dariane, C.; de la Rosette, J. Advanced Ultrasound in the Diagnosis of Prostate Cancer. World J Urol 2021, 39, 661–676, doi:10.1007/s00345-020-03193-0.
CrossRef - Clements, A.; Watson, E.; Rai, T.; Bukach, C.; Shine, B.; Austoker, J. The PSA Testing Dilemma: GPs’ Reports of Consultations with Asymptomatic Men: A Qualitative Study. BMC Fam Pract 2007, 8, 35, doi:10.1186/1471-2296-8-35.
CrossRef - Hayes, J.H.; Barry, M.J. Screening for Prostate Cancer With the Prostate-Specific Antigen Test. JAMA 2014, 311, 1143, doi:10.1001/jama.2014.2085.
CrossRef - Moyer, V.A. Screening for Prostate Cancer: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med 2012, 157, 120, doi:10.7326/0003-4819-157-2-201207170-00459.
CrossRef - Prashant Koppuravuri, N.; Sai Bharath, V.M.; Yunus Pasha, T. Car-T Cell Therapy for Cancer: A Review. Author Advances in Bioresearch Adv. Biores 2023, 14, 354–360, doi:10.15515/abr.0976-4585.14.4.354360.
- Manojmouli, C.; Pasha, T.Y.; Nagaprashant, K.; Ramesh, B.; Ul Eain, N.; Purushotham, K.N. Flavonoid Derivatives as Anticancer Moiety and Its Effect on Cancer Cell Lines: An Updated Review. Journal of the Serbian Chemical Society 2023, 88, 937–957, doi:10.2298/JSC221228041M.
CrossRef - Pasha, T.Y.; Manojmouli, C.; Ramesh, B.; Prashant, K.N.; Purushotham, K.N.; Eain, N.U.; Shankar, M. Therapeutic Importance of Biological Half-Life of Antineoplastic Agents- A Review. Advances in Pharmacology and Pharmacy 2022, 10, 265–272, doi:10.13189/app.2022.100405.
CrossRef - Litwin, M.S.; Tan, H.-J. The Diagnosis and Treatment of Prostate Cancer. JAMA 2017, 317, 2532, doi:10.1001/jama.2017.7248.
CrossRef - Teo, M.Y.; Rathkopf, D.E.; Kantoff, P. Treatment of Advanced Prostate Cancer. Annu Rev Med 2019, 70, 479–499, doi:10.1146/annurev-med-051517-011947.
CrossRef - Klotz, L.; Vesprini, D.; Sethukavalan, P.; Jethava, V.; Zhang, L.; Jain, S.; Yamamoto, T.; Mamedov, A.; Loblaw, A. Long-Term Follow-Up of a Large Active Surveillance Cohort of Patients With Prostate Cancer. Journal of Clinical Oncology 2015, 33, 272–277, doi:10.1200/JCO.2014.55.1192.
CrossRef - van den Bergh, R.C.N.; Roemeling, S.; Roobol, M.J.; Aus, G.; Hugosson, J.; Rannikko, A.S.; Tammela, T.L.; Bangma, C.H.; Schröder, F.H. Outcomes of Men with Screen-Detected Prostate Cancer Eligible for Active Surveillance Who Were Managed Expectantly. Eur Urol 2009, 55, 1–8, doi:10.1016/j.eururo.2008.09.007.
CrossRef - Cooperberg, M.R.; Carroll, P.R.; Klotz, L. Active Surveillance for Prostate Cancer: Progress and Promise. Journal of Clinical Oncology 2011, 29, 3669–3676, doi:10.1200/JCO.2011.34.9738.
CrossRef - Romero‐Otero, J.; García‐Gómez, B.; Duarte‐Ojeda, J.M.; Rodríguez‐Antolín, A.; Vilaseca, A.; Carlsson, S. V; Touijer, K.A. Active Surveillance for Prostate Cancer. International Journal of Urology 2016, 23, 211–218, doi:10.1111/iju.13016.
CrossRef - Sebesta, E.M.; Anderson, C.B. The Surgical Management of Prostate Cancer. Semin Oncol 2017, 44, 347–357, doi:10.1053/j.seminoncol.2018.01.003.
CrossRef - Chen, F.; Zhao, X. Prostate Cancer: Current Treatment and Prevention Strategies. Iran Red Crescent Med J 2013, 15, 279–284, doi:10.5812/ircmj.6499.
CrossRef - Wilkins, L.J.; Tosoian, J.J.; Sundi, D.; Ross, A.E.; Grimberg, D.; Klein, E.A.; Chapin, B.F.; Nyame, Y.A. Surgical Management of High-Risk, Localized Prostate Cancer. Nat Rev Urol 2020, 17, 679–690, doi:10.1038/s41585-020-00384-7.
CrossRef - Baskar, R.; Lee, K.A.; Yeo, R.; Yeoh, K.-W. Cancer and Radiation Therapy: Current Advances and Future Directions. Int J Med Sci 2012, 9, 193–199, doi:10.7150/ijms.3635.
CrossRef - Quinn, D.I.; Sandler, H.M.; Horvath, L.G.; Goldkorn, A.; Eastham, J.A. The Evolution of Chemotherapy for the Treatment of Prostate Cancer. Annals of Oncology 2017, 28, 2658–2669, doi:10.1093/annonc/mdx348.
CrossRef - Nevedomskaya, E.; Baumgart, S.J.; Haendler, B. Recent Advances in Prostate Cancer Treatment and Drug Discovery. Int J Mol Sci 2018, 19, 1359, doi:10.3390/ijms19051359.
CrossRef - Nader, R.; El Amm, J.; Aragon-Ching, J. Role of Chemotherapy in Prostate Cancer. Asian J Androl 2018, 20, 221, doi:10.4103/aja.aja_40_17.
CrossRef - Fay, E.K.; Graff, J.N. Immunotherapy in Prostate Cancer. Cancers (Basel) 2020, 12, 1752, doi:10.3390/cancers12071752.
CrossRef - Cha, H.-R.; Lee, J.H.; Ponnazhagan, S. Revisiting Immunotherapy: A Focus on Prostate Cancer. Cancer Res 2020, 80, 1615–1623, doi:10.1158/0008-5472.CAN-19-2948.
CrossRef - Handa, S.; Hans, B.; Goel, S.; Bashorun, H.O.; Dovey, Z.; Tewari, A. Immunotherapy in Prostate Cancer: Current State and Future Perspectives. Ther Adv Urol 2020, 12, doi:10.1177/1756287220951404.
CrossRef - Abeshouse, A.; Ahn, J.; Akbani, R.; Ally, A.; Amin, S.; Andry, C.D.; Annala, M.; Aprikian, A.; Armenia, J.; Arora, A.; et al. The Molecular Taxonomy of Primary Prostate Cancer. Cell 2015, 163, 1011–1025, doi:10.1016/j.cell.2015.10.025.
CrossRef - Parker, C.; Castro, E.; Fizazi, K.; Heidenreich, A.; Ost, P.; Procopio, G.; Tombal, B.; Gillessen, S. Prostate Cancer: ESMO Clinical Practice Guidelines for Diagnosis, Treatment and Follow-Up. Annals of Oncology 2020, 31, 1119–1134, doi:10.1016/j.annonc.2020.06.011.
CrossRef - Resnick, M.J.; Koyama, T.; Fan, K.-H.; Albertsen, P.C.; Goodman, M.; Hamilton, A.S.; Hoffman, R.M.; Potosky, A.L.; Stanford, J.L.; Stroup, A.M.; et al. Long-Term Functional Outcomes after Treatment for Localized Prostate Cancer. New England Journal of Medicine 2013, 368, 436–445, doi:10.1056/NEJMoa1209978.
CrossRef
Accepted on: 17 Mar 2025
Second Review by: Dr. Anjana Male
Final Approval by: Dr. Ioana Stanciu

















